The once-dramatic notion of doctors declaring “no options left” for common bacterial infections is rapidly transforming into a grim reality for a growing number of individuals. This alarming shift is propelled by the escalating global crisis of antibiotic resistance. A tragic testament to this intensifying danger occurred in 2016, when a woman from Nevada succumbed to a bacterial infection that proved resistant to all 26 antibiotics then available in the United States.
Antimicrobial resistance (AMR) poses a profound global health threat, with stark figures illustrating its devastating reach. In the United States, more than 2.8 million antibiotic-resistant illnesses are reported annually. On a global scale, the crisis deepens dramatically, with AMR now linked to a staggering nearly 5 million deaths each year.
Here are a few options for paraphrasing the text, maintaining a clear, journalistic tone:
**Option 1 (Focus on cause and effect):**
> Bacteria naturally evolve to overcome drug treatments, inherently developing resistance that renders medications less effective. However, the improper and excessive use of antibiotics, both in human medicine and agricultural settings, drastically accelerates this evolutionary process, significantly hastening the emergence of drug-resistant strains.
**Option 2 (Highlighting human impact):**
> While bacteria possess an innate ability to adapt and gradually circumvent the effectiveness of antimicrobial drugs, it is the widespread misuse and overuse of antibiotics—in healthcare and agriculture alike—that truly supercharges the development of resistance. This human-driven pressure transforms a slow, natural adaptation into a rapidly escalating threat.
**Option 3 (Concise and direct):**
> The natural evolutionary pathways of bacteria inherently lead to diminished drug efficacy. Yet, this organic process is severely compounded and accelerated by the inappropriate and excessive application of antibiotics across medical and agricultural sectors, fueling the rapid rise of resistant strains.
Modern medicine is confronting an urgent and escalating crisis as the relentless spread of antibiotic-resistant bacteria fundamentally complicates life-saving treatments. What were once considered common infections are now proving stubbornly difficult to overcome, while the inherent risks associated with routine surgical procedures are alarmingly elevated.
Counteracting this profound threat demands a multi-pronged, collective effort. It extends beyond the crucial practices of judicious antibiotic use and robust hygiene protocols. A critical component is also fostering widespread public awareness of how individual, everyday actions inadvertently fuel the rise of these “superbugs” and impact global health.
The specter of drug resistance has haunted medicine since 1910, the very year Salvarsan, the pioneering synthetic antibiotic for syphilis, made its debut. More than a century later, a prominent microbiologist and biochemist specializing in antimicrobial resistance has now outlined four pivotal trends. These, the expert asserts, are poised to fundamentally redefine how societies worldwide will confront the escalating challenge of antibiotic resistance over the next decade.
For years, medical professionals have navigated the challenge of bacterial infections with a degree of informed estimation. When critically ill patients present at a hospital, and the specific pathogen causing their illness has not yet been definitively identified, clinicians often initiate treatment with broad-spectrum antibiotics.
This immediate, wide-ranging antimicrobial approach can be crucial and potentially life-saving, as these drugs are designed to eliminate a diverse array of bacterial types simultaneously. However, this strategy also inevitably exposes a vast population of other bacteria within the body—including harmless or beneficial microbes—to the antibiotic.
While the intended pathogenic bacteria might be neutralized, the surviving bacteria, now under selective pressure, continue to multiply. Crucially, they can also exchange genes that confer resistance, effectively enabling other bacterial species to evade the drug. This widespread, often unnecessary, exposure inadvertently provides an opportunity for various bacteria to adapt and develop drug resistance, escalating a critical public health challenge.
Here are a few paraphrased options, maintaining a journalistic tone:
**Option 1 (Focus on clinician dilemma):**
> While narrow-spectrum antibiotics offer the advantage of precisely targeting a limited range of bacteria, thus preserving beneficial microbial communities, their application is often hampered by diagnostic delays. Clinicians frequently find themselves compelled to initiate broad-spectrum treatment for critically ill patients, as identifying the specific pathogen responsible for an infection can take several days, leaving them with few immediate therapeutic alternatives.
**Option 2 (More concise and direct):**
> Unlike their broader counterparts, narrow-spectrum antibiotics zero in on a specific set of bacteria, a characteristic favored by medical professionals for their ability to combat infection without disrupting the body’s natural bacterial balance. The significant hurdle, however, lies in the time-consuming process of pinpointing the exact culprit. This waiting period often forces clinicians to default to broad-spectrum antibiotics, particularly when a patient’s condition is severe.
**Option 3 (Emphasizing the “why” behind broad-spectrum use):**
> The precision of narrow-spectrum antibiotics, which confine their action to a select group of bacteria, is often preferred by clinicians for their targeted approach to infection control. However, the practical challenge of swiftly identifying the precise bacterial agent frequently leads to the preemptive use of broad-spectrum antibiotics. This is especially common in cases involving seriously ill patients, where the immediate need to intervene outweighs the diagnostic uncertainty.
**Rapid, On-Site Diagnostics Poised to Revolutionize Bacterial Infection Treatment**
Cutting-edge technologies are on the horizon to significantly accelerate the identification of bacterial pathogens, potentially bringing diagnostic capabilities directly to the patient’s bedside. This advancement promises to eliminate the lengthy delays associated with traditional off-site sample analysis, offering near-instantaneous results.
Fueled by breakthroughs in genomic sequencing, microfluidics, and artificial intelligence, medical professionals may soon be able to pinpoint specific bacterial species and determine the most effective antibiotic treatments within mere hours, a dramatic improvement from the days previously required. Furthermore, sophisticated predictive tools are emerging that can forecast the evolution of antibiotic resistance, empowering clinicians to stay ahead of this critical challenge.
Here are a few paraphrased options, each with a slightly different emphasis, maintaining a professional, journalistic tone:
**Option 1 (Focus on clinician benefit and research imperative):**
> Enhanced diagnostic tools offer clinicians a pathway to quicker, more accurate diagnoses and treatment strategies that actively combat the rise of drug resistance. Simultaneously, these advancements highlight a critical imperative for researchers to connect diagnostic capabilities with real-time surveillance systems designed to monitor evolving resistance patterns as they surface.
**Option 2 (More concise, action-oriented):**
> For healthcare providers, improved tests promise accelerated diagnoses and treatment plans that minimize the risk of worsening drug resistance. Researchers, in turn, are prompted by these tools to urgently integrate diagnostics into live surveillance networks, enabling the tracking of emerging resistance trends.
**Option 3 (Emphasizing the dual role of the tools):**
> These superior diagnostic tests serve a dual purpose: empowering clinicians with faster diagnoses and more effective, resistance-aware treatment plans, while simultaneously underscoring for researchers the vital necessity of linking diagnostic technologies with real-time surveillance networks capable of charting the emergence of resistance patterns.
**Option 4 (Slightly more descriptive):**
> The development of more sophisticated diagnostic tests holds significant promise for clinicians, enabling them to arrive at diagnoses more swiftly and devise treatment plans that are both effective and designed to prevent the amplification of resistance. For the research community, these new tools underscore a pressing need to embed diagnostics within dynamic surveillance networks that can diligently track resistance trends as they develop.
Choose the option that best fits the specific context and desired nuance for your writing.
Here are a few paraphrased options, keeping a clear, journalistic tone and emphasizing the original meaning:
**Option 1 (Focus on enabling action):**
> While not a complete solution on their own, diagnostics offer the crucial precision, speed, and early detection necessary to proactively combat resistance.
**Option 2 (Highlighting the strategic advantage):**
> Diagnostics are a vital component in the fight against resistance, providing the speed, accuracy, and early warning system that allows for a strategic advantage.
**Option 3 (Emphasizing preventative power):**
> The power of diagnostics lies in their ability to deliver the precision, speed, and early alerts essential for anticipating and addressing resistance before it becomes a crisis.
**Option 4 (More direct and concise):**
> Diagnostics alone won’t eradicate resistance, but they are indispensable for delivering the speed, accuracy, and early detection needed to stay a step ahead.
**Key changes and why they work:**
* **”Solve resistance” vs. “combat resistance,” “eradicate resistance,” “address resistance,” “stay ahead,” “proactively combat”:** These phrases offer variety and more active or strategic connotations.
* **”Provide the precision, speed and early warning needed” vs. “offer the crucial precision, speed, and early detection necessary,” “providing the speed, accuracy, and early warning system that allows for a strategic advantage,” “deliver the precision, speed, and early alerts essential,” “delivering the speed, accuracy, and early detection needed”:** These rephrased clauses maintain the core benefits while using different vocabulary and sentence structures.
* **”Stay ahead” vs. “proactively combat,” “strategic advantage,” “anticipating and addressing resistance before it becomes a crisis,” “stay a step ahead”:** These options create a stronger sense of forward-thinking and control.
* **Journalistic Tone:** The language is direct, factual, and avoids overly technical jargon or flowery language.
Here are a few paraphrased options, each with a slightly different nuance, maintaining a journalistic tone:
**Option 1 (Focus on the current challenge):**
> While antibiotics revolutionized 20th-century healthcare, their continued efficacy into the 21st century is far from guaranteed. A critical shortage of novel antibiotic development persists, with the majority of drugs in the current pipeline offering only minor variations on existing treatments, raising concerns about their long-term impact.
**Option 2 (More direct and urgent):**
> The medical landscape of the 20th century was reshaped by antibiotics, yet this reliance is proving insufficient for the challenges of the 21st. The development of new antibiotic drugs has slowed to an alarming degree, and many in the current research pipeline are too similar to established medications to offer a significant breakthrough.
**Option 3 (Emphasizing the need for innovation):**
> Antibiotics stand as a cornerstone of 20th-century medical progress, but humanity cannot depend solely on these existing tools to navigate the health crises of the 21st. The flow of truly new antibiotic development is worryingly limited, and the drugs currently under consideration largely mimic existing compounds, potentially undermining their future effectiveness.
**Option 4 (Concise and impactful):**
> The transformative power of 20th-century antibiotics is undeniable, but their singular dominance is insufficient for the 21st century. A concerning scarcity of new antibiotic development plagues the medical field, with most emerging drugs offering little structural innovation beyond existing treatments, thus limiting their potential impact.
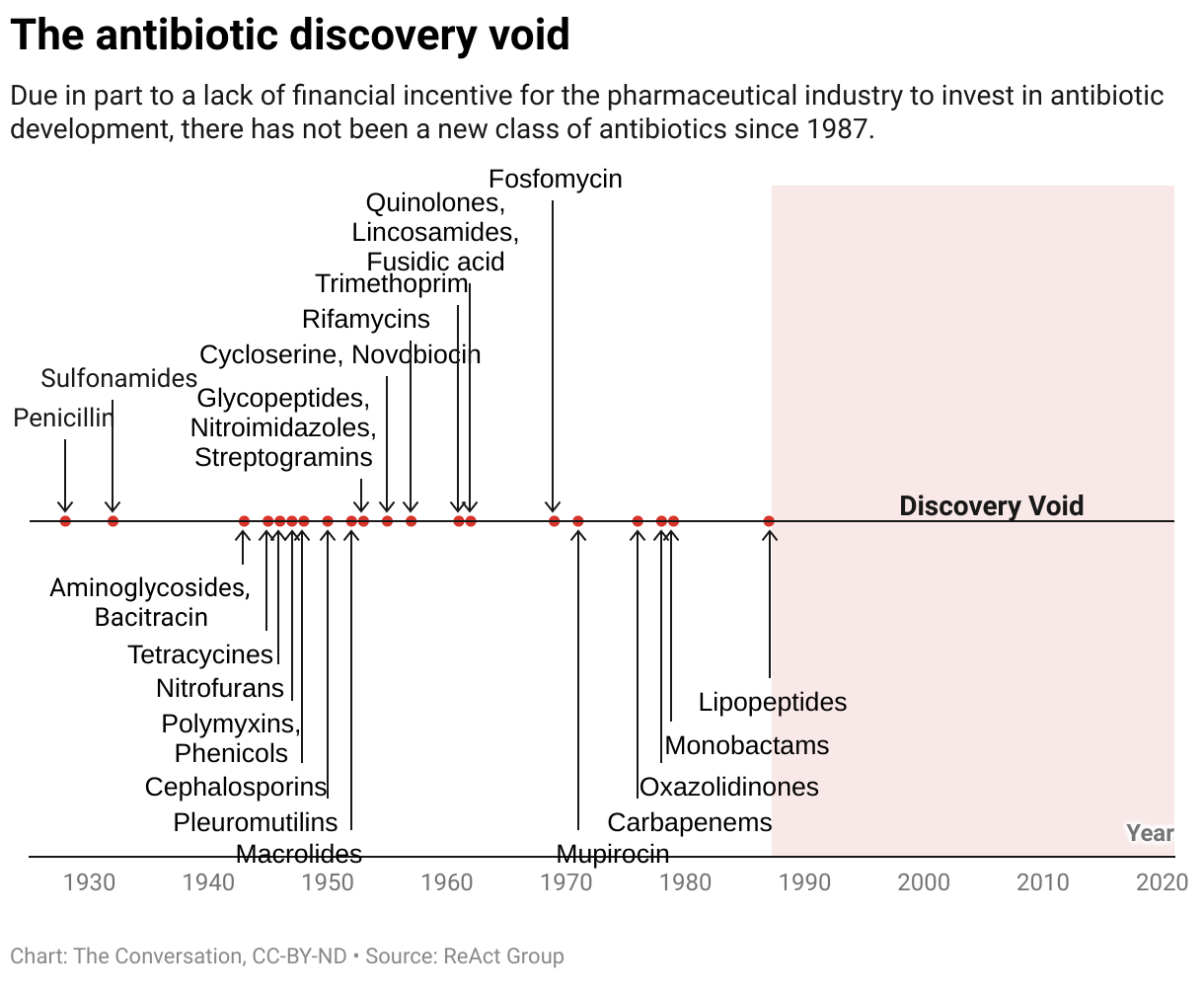
## A Troubling Gap in Our Arsenal Against Bacteria: The Antibiotic Discovery Drought
For decades, the world has relied on a powerful arsenal of antibiotics to combat bacterial infections, saving countless lives and revolutionizing modern medicine. However, a concerning reality has emerged: we are facing a critical **antibiotic discovery void**. The pipeline for new life-saving drugs is drying up, leaving us increasingly vulnerable to the growing threat of antibiotic-resistant bacteria.
This “void” signifies a significant slowdown in the development and introduction of novel antibiotics. For years, the rate at which we discover and bring new classes of these essential medicines to market has dwindled. This isn’t a sudden crisis, but rather a decades-long trend that has left us with a limited and aging repertoire of drugs to combat an ever-evolving enemy.
The implications are stark. As bacteria become more adept at evading current treatments, infections that were once easily managed are becoming harder to treat, leading to longer illnesses, increased mortality rates, and soaring healthcare costs. Without a renewed surge in antibiotic innovation, the very foundations of modern healthcare – from routine surgeries to cancer chemotherapy – could be jeopardized. Understanding the reasons behind this discovery drought is crucial to charting a path forward and ensuring we don’t lose our critical battle against bacterial threats.
Here are a few paraphrased options, playing with slightly different angles and tones while keeping the journalistic style:
**Option 1 (Focus on innovation):**
> In a race to stay ahead of evolving pathogens, scientists are channeling resources into a new wave of experimental therapies. These innovative approaches often diverge significantly from conventional antibiotic mechanisms, offering entirely novel ways to combat infections.
**Option 2 (Focus on the “different ways”):**
> Pushing the boundaries of infectious disease treatment, researchers are exploring a variety of unconventional therapies. These novel strategies frequently operate on principles distinct from established antibiotics, promising a new arsenal against stubborn microbial threats.
**Option 3 (More direct and concise):**
> To maintain a leading edge in combating infections, researchers are increasingly backing nontraditional therapies. Many of these cutting-edge treatments employ mechanisms of action that fundamentally differ from those of standard antibiotics.
**Option 4 (Slightly more evocative):**
> The pursuit of effective infection control is leading researchers down new paths, with significant investment in therapies that break from tradition. These innovative treatments are designed to work in ways fundamentally unlike our current antibiotic arsenal, signaling a shift in strategy.
Choose the option that best fits the specific context and emphasis you want to convey.
Here are a few paraphrased options, each with a slightly different emphasis:
**Option 1 (Focus on Action):**
> A promising avenue for combating bacterial infections involves bacteriophage therapy, a method that deploys viruses engineered to target and eliminate specific harmful bacteria. Concurrently, researchers are developing microbiome-based treatments aimed at re-establishing beneficial bacterial populations to effectively displace disease-causing pathogens.
**Option 2 (Focus on Innovation):**
> Innovative approaches are emerging in the fight against bacteria, including bacteriophage therapy, which harnesses viruses to precisely infect and destroy detrimental bacterial strains. Another innovative direction involves microbiome-based interventions designed to cultivate healthy bacterial ecosystems, thereby outcompeting and suppressing harmful microbes.
**Option 3 (More Concise):**
> Promising strategies include bacteriophage therapy, utilizing viruses to kill specific harmful bacteria, and microbiome-based treatments that restore healthy bacterial communities to naturally combat pathogens.
**Option 4 (Slightly More Detailed):**
> Among the most promising strategies for tackling bacterial threats is bacteriophage therapy, a treatment that employs viruses with a remarkable ability to target and destroy specific types of harmful bacteria. In parallel, scientists are investigating microbiome-based therapies, which focus on rebuilding balanced communities of beneficial bacteria to naturally inhibit the growth and spread of pathogens.
**Key changes made across these options:**
* **Synonyms:** “Promising direction” becomes “promising avenue,” “innovative approaches,” “promising strategies.” “Specifically infect and kill” becomes “target and eliminate,” “precisely infect and destroy,” “remarkable ability to target and destroy.” “Harmful bacteria” becomes “detrimental bacterial strains,” “disease-causing pathogens,” “harmful microbes.” “Restore healthy bacterial communities” becomes “re-establishing beneficial bacterial populations,” “cultivate healthy bacterial ecosystems,” “rebuilding balanced communities of beneficial bacteria.” “Crowd out pathogens” becomes “displace pathogens,” “outcompeting and suppressing pathogens,” “naturally combat pathogens,” “inhibit the growth and spread of pathogens.”
* **Sentence Structure:** Varied sentence beginnings and clause arrangements.
* **Active Voice:** Generally favored to make the writing more direct.
* **Journalistic Tone:** Employed clear, objective language.
**Innovative antimicrobial strategies are emerging, leveraging cutting-edge technologies to combat drug-resistant infections.** Scientists are harnessing the precision of CRISPR gene-editing to target and neutralize the very genes that confer antibiotic resistance in bacteria.
Beyond gene editing, **novel therapeutic agents are on the horizon, including antimicrobial peptides.** These potent molecules work by physically disrupting bacterial cell membranes, offering a distinct mechanism of action against resistant microbes.
Furthermore, **advances in drug delivery are poised to revolutionize treatment efficacy.** Researchers are developing sophisticated nanoparticle systems designed to ferry antimicrobial compounds directly to the site of infection. This targeted approach promises to enhance drug concentration where it’s needed most, while simultaneously minimizing off-target side effects for patients.
Scientists are exploring innovative, non-medical strategies to curb the spread of antibiotic resistance genes. These efforts are focused on interrupting gene transfer pathways in environments such as soil, wastewater, and even within plastic materials, in addition to vital aquatic ecosystems and other natural reservoirs.
Here are a few options for paraphrasing the provided text, each with a slightly different emphasis:
**Option 1 (Focus on the Shift in Strategy):**
> While many of these emerging strategies are still in their infancy and face the potential challenge of bacterial adaptation, they signal a significant change in approach. The scientific community is moving away from the singular pursuit of new antibiotics to combat resistance, instead focusing on developing a multifaceted and robust arsenal of tools to tackle drug-resistant pathogens.
**Option 2 (More Direct and Action-Oriented):**
> These promising avenues are largely in their early phases, and bacteria could eventually develop ways to circumvent them. Nevertheless, these advancements highlight a crucial pivot: rather than relying on the discovery of a single magic bullet antibiotic, researchers are now cultivating a broader and more adaptable suite of defenses against antibiotic-resistant bacteria.
**Option 3 (Emphasizing Diversity and Resilience):**
> Though many of these innovations are nascent and bacteria may ultimately find ways to overcome them, they represent a powerful evolution in our fight against antibiotic resistance. The focus has shifted from a gamble on discovering a solitary antibiotic to the strategic construction of a more diverse and resilient toolkit capable of outmaneuvering drug-resistant pathogens.
**Option 4 (Concise and Journalistic):**
> These emerging solutions are largely experimental, and bacterial evolution remains a persistent threat. However, these innovations underscore a significant shift in strategy: researchers are no longer solely pursuing the discovery of a single antibiotic, but are instead building a diverse and resilient arsenal to combat antibiotic-resistant bacteria.
Each of these options aims to:
* **Maintain the core meaning:** The shift from a single-antibiotic focus to a diverse toolkit is preserved.
* **Be unique and original:** Different sentence structures, vocabulary, and phrasing are used.
* **Be engaging:** Words like “emerging strategies,” “significant change,” “crucial pivot,” and “powerful evolution” aim to capture reader interest.
* **Use a clear, journalistic tone:** The language is direct, informative, and avoids overly technical jargon.
Antibiotic resistance is far from being solely a hospital-based problem; its reach extends significantly beyond clinical environments. This pervasive threat spreads across a complex web of pathways, involving human populations, wildlife, agricultural crops, wastewater systems, soil, and intricate global trade networks. To accurately grasp how resistance genes navigate these diverse ecosystems, adopting a comprehensive “One Health” perspective is not merely beneficial, but absolutely essential. This broader understanding is critical for effectively monitoring and combating the multifaceted challenge of antibiotic resistance.
A critical shift in scientific understanding reveals that environmental and agricultural practices are emerging as major drivers of antibiotic resistance, now considered on par with the long-recognized problem of clinical misuse.
This expanding recognition highlights several critical pathways for resistance proliferation. For instance, the widespread application of antibiotics in animal agriculture directly fosters the development of resistant bacterial strains capable of transmitting to human populations. Compounding this, antibiotic resistance genes present in wastewater streams often evade traditional treatment systems, subsequently contaminating rivers and agricultural soils. Consequently, specific ‘environmental hotspots’—such as farms and sewage treatment facilities—act as crucial nexus points where resistance can proliferate at an accelerated rate. Further exacerbating the global challenge, international travel rapidly transports these resistant bacteria across continents, often within mere hours, underscoring the urgent need for a holistic approach to containment.
The expanding threat of antibiotic resistance reaches far beyond clinical settings, revealing itself as a profound ecological and societal challenge. Addressing this complex problem demands an unprecedented interdisciplinary approach from researchers, requiring the seamless integration of insights from fields such as microbiology, ecology, engineering, agriculture, and public health to develop effective solutions.
Developing new antibiotics, a critical endeavor for global health, presents a significant and often insurmountable financial challenge for pharmaceutical companies. Paradoxically, the very strategies designed to preserve the effectiveness of these life-saving drugs undermine their market viability.
To combat the escalating threat of antimicrobial resistance, novel antibiotics are intentionally used sparingly, limiting their deployment to essential cases. While medically prudent, this cautious approach drastically restricts the volume of doses sold. Consequently, even after receiving crucial Food and Drug Administration approval, many companies struggle to generate sufficient revenue to recoup their extensive research and development expenditures. This inherent economic imbalance has already driven several promising antibiotic developers into bankruptcy, highlighting a critical market failure within the pharmaceutical industry.
In a significant move to stimulate the development of urgently needed new antibiotics, the United States is actively exploring major policy reforms, chief among them the bipartisan PASTEUR Act. This proposed legislation aims to revolutionize how drug manufacturers are compensated by introducing a “subscription-style” payment model. Under this innovative system, the federal government could allocate up to US$3 billion over a five-to-ten-year period to secure access to critical antibiotics, fundamentally shifting away from the conventional per-pill payment method and directly incentivizing innovation in antibiotic research and production.
Leading international health organizations, spearheaded by Médecins Sans Frontières (Doctors Without Borders), are emphasizing that the proposed bill must integrate more robust commitments to diligent stewardship and truly equitable access for all.
This legislation marks a pivotal moment in the fight against antimicrobial resistance in the United States, potentially shaping the very availability of antibiotics for years to come.
Here are a few paraphrased options, maintaining a clear, journalistic tone and focusing on a hopeful outlook:
**Option 1 (Concise & Direct):**
> Contrary to fears of an unavoidable crisis, the fight against antibiotic resistance is entering a more optimistic phase. Experts anticipate a future bolstered by advanced diagnostics, novel treatments, comprehensive ecosystem-wide approaches, and policy shifts designed not only to promote responsible antibiotic use but also to revitalize the development of new drugs.
**Option 2 (Slightly More Elaborate):**
> The narrative surrounding antibiotic resistance, often painted as an impending doom, is shifting towards a more hopeful outlook. We are witnessing the dawn of an era characterized by sophisticated diagnostic tools, groundbreaking therapeutic interventions, and broad strategies that consider the entire ecosystem. Crucially, this period will also be marked by policy reforms aimed at both improving antibiotic stewardship and reigniting the crucial pipeline for developing new life-saving medications.
**Option 3 (Focus on Action & Progress):**
> While the specter of antibiotic resistance looms, a more positive trajectory is emerging. This shift signifies a move beyond an inevitable catastrophe towards proactive solutions. The coming era promises advancements in intelligent diagnostics, the development of innovative therapies, a holistic, ecosystem-level approach to tackling resistance, and essential policy reforms. These initiatives are poised to simultaneously enhance antibiotic stewardship and rebuild the critical pipeline for antibiotic development.
**Key changes made and why:**
* **”Inevitability” vs. “Hopeful reality”:** The original phrasing is directly addressed and countered with stronger, more active language like “optimistic phase,” “hopeful outlook,” and “positive trajectory.”
* **”Entering an era”:** Rephrased as “entering a more optimistic phase,” “dawn of an era,” or “coming era” to inject a sense of progression and forward momentum.
* **”Smarter diagnostics, innovative therapies, ecosystem-level strategies and policy reforms”:** These are kept as the core elements but are often introduced with more descriptive adjectives or framed as “advancements” and “interventions.”
* **”Rebuilding the antibiotic pipeline in addition to addressing stewardship”:** This crucial dual focus is maintained but articulated with variations like “revitalize the development of new drugs,” “reigniting the crucial pipeline for developing new life-saving medications,” or “simultaneously enhance antibiotic stewardship and rebuild the critical pipeline.”
* **Journalistic Tone:** Achieved through clear sentence structure, objective language (while conveying optimism), and a focus on societal shifts and expert perspectives.
* **Engagement:** Using words like “bolstered,” “groundbreaking,” “crucially,” and “poised” adds a layer of dynamism and reader interest.
Here are a few ways to paraphrase that sentence, depending on the desired nuance:
**Option 1 (Focus on tangible benefits):**
> This advancement translates into enhanced tools and more robust safeguards for the public, while simultaneously fostering novel avenues of collaboration between researchers and policymakers.
**Option 2 (Focus on enhanced capabilities):**
> Citizens can now expect superior tools and fortified protective measures, a development that necessitates innovative partnerships and cooperative efforts among researchers and policymakers.
**Option 3 (More concise and direct):**
> The public will benefit from improved tools and stronger protections, prompting researchers and policymakers to engage in new forms of collaboration.
**Option 4 (Emphasizing the dual nature of the impact):**
> On one hand, this signifies an upgrade in protective tools and systems for the general populace. On the other, it calls for a redefinition of collaborative practices between the research and policy communities.
Here are a few paraphrased options, each with a slightly different emphasis, while maintaining a journalistic tone:
**Option 1 (Focus on Urgency):**
> The critical juncture has arrived: the debate has shifted from identifying cures for antibiotic resistance to determining if humanity can implement these solutions with sufficient speed.
**Option 2 (More Direct and Concise):**
> The challenge of antibiotic resistance has moved beyond finding answers; the pressing question is whether society will mobilize quickly enough to deploy existing remedies.
**Option 3 (Emphasizing the Societal Aspect):**
> We are no longer debating the existence of solutions to the escalating threat of antibiotic resistance. Instead, the crucial question centers on society’s capacity and willingness to act decisively and promptly.
**Option 4 (Slightly More Dramatic):**
> The era of questioning potential fixes for antibiotic resistance is over. The urgent concern now is whether collective action will keep pace with the rapid spread of the problem.
Each of these options aims to convey the same core message: the solutions exist, but the race is against time and societal inertia.
Here are a few ways to rephrase “This edited article is republished from The Conversation under a Creative Commons license. Read the original article.” in a journalistic tone, offering slightly different nuances:
**Option 1 (Concise and direct):**
> This piece, originally published by The Conversation, is being shared here under a Creative Commons license. You can find the full, original article [link to original article].
**Option 2 (Slightly more informative):**
> As a republication from The Conversation, this article is made available under a Creative Commons license. For the complete original content, please refer to [link to original article].
**Option 3 (Emphasizing the source):**
> Sourced from The Conversation, this article is presented here with a Creative Commons license. The original publication can be accessed at [link to original article].
**Option 4 (Highlighting the licensing):**
> With permission from The Conversation, this article is republished under a Creative Commons license. The original version is available for review at [link to original article].
**Key changes and why they work journalistically:**
* **”This edited article” becomes “This piece,” “This article,” or “This item”**: More common journalistic phrasing. “Edited” can sometimes imply a reduction in quality, which might not be the intended message.
* **”is republished from” becomes “originally published by,” “As a republication from,” or “Sourced from”**: These are more active and engaging verbs.
* **”under a Creative Commons license” remains similar**: This is a factual statement that needs to be clear.
* **”Read the original article” becomes a more formal call to action like “You can find the full, original article,” “For the complete original content, please refer to,” or “The original publication can be accessed at”**: These are more professional ways to direct readers.
* **Adding “[link to original article]”**: Crucial for journalistic practice, it’s essential to provide a direct path to the source.
Choose the option that best fits the overall tone and style of the platform where this information will be presented.







