In just one year, Secretary of Health and Human Services Robert F. Kennedy Jr. (RFK Jr.) has significantly weakened the nation’s highly effective HIV prevention program. This extensive disruption, critics contend, has left the country alarmingly exposed to a burgeoning HIV pandemic, a concerning development given that the complete eradication of HIV had previously appeared to be a tangible possibility.
Recent developments have sent shockwaves through the HIV community, leaving many professionals deeply concerned and apprehensive. Yet, drawing on personal experience, I am convinced that a potent combination of robust scientific inquiry and unwavering advocacy holds the key. This synergy, I believe, can decisively steer us back onto the critical path toward achieving HIV elimination.
The genesis of the AIDS epidemic unfolded directly before my eyes. In 1983, during my final year of medical school, I gained firsthand insight into the emerging crisis through a month-long practice internship at San Francisco General Hospital. This institution housed the nation’s first dedicated AIDS ward, a pioneering effort in the face of a terrifying new disease. At that critical juncture, the medical community grappled with profound unknowns: the very cause of Acquired Immunodeficiency Syndrome (AIDS) remained a mystery, no diagnostic tests were available, effective treatments were non-existent, and even the basic understanding of its transmission modes was a subject of intense and often controversial debate.
In its initial surge, the epidemic disproportionately affected gay men, with confirmed AIDS diagnoses escalating at an alarming rate. Those afflicted faced protracted and agonizing deaths. The disease exacted a horrific physical toll, manifesting in blindness, severe emaciation, persistent vomiting, respiratory failure, and widespread lesions. Compounding the medical and personal suffering was profound social isolation, as pervasive fear of contagion often led to abandonment by neighbors, family, and friends.
In the wake of the pivotal Stonewall Riots and the assassination of pioneering LGBTQ+ activist Harvey Milk, the devastating arrival of the AIDS epidemic ushered in a new era of moral condemnation. From their pulpits across the nation, fundamentalist preachers swiftly seized upon the tragedy, proclaiming the disease to be God’s righteous judgment, a justified vengeance against those they labeled ‘sinners’.
Another prevailing viewpoint favored a quiet, low-resource, and hands-off approach, implicitly suggesting that the AIDS epidemic served as a natural mechanism to eliminate those deemed “undesirable.”
In the wake of early observations within AIDS wards, researchers swiftly pinpointed the devastating illness’s origin: the human immunodeficiency virus (HIV).
**Groundbreaking activism, bolstered by scientific understanding, transformed HIV/AIDS from a death sentence into a manageable condition.** In the face of a devastating epidemic, dedicated activists challenged the prevailing narrative and spearheaded a powerful movement advocating for urgent research into treatments. Their relentless efforts yielded remarkable results, leading to the rapid development of a diverse array of anti-HIV medications. This therapeutic revolution has profoundly altered the landscape of the disease, enabling the vast majority of individuals living with HIV to achieve near-normal life expectancies.
Here are a few paraphrased options, each with a slightly different emphasis, while maintaining a journalistic tone:
**Option 1 (Focus on the core discovery):**
> Ironically, progress in extending the lives of those with HIV inadvertently fueled the epidemic’s growth. In 2010, while stationed with the Centers for Disease Control and Prevention (CDC) in Kenya, I played a minor part in a massive, international research effort. This study aimed to determine if antiretroviral therapy could be leveraged to prevent the spread of HIV. My role involved briefing healthcare professionals at the local public hospital, who would be instrumental in implementing this groundbreaking study and related initiatives.
**Option 2 (More active voice, highlighting the paradox):**
> A surprising paradox emerged from advancements in HIV treatment: Longer lifespans for infected individuals led to a widening epidemic. In 2010, I was part of the CDC’s HIV prevention efforts in Kenya. My work included a small but crucial contribution to a vast multinational study investigating the potential of antiretroviral drugs to halt HIV transmission. During a meeting at the local public hospital, I addressed a group of healthcare workers tasked with executing this and similar research projects.
**Option 3 (Concise and direct):**
> The effectiveness of HIV treatments created a paradoxical situation: increased life expectancy for infected individuals corresponded with an expanding epidemic. In 2010, my work with the CDC on HIV prevention in Kenya involved a modest role in a substantial multinational study. This research sought to confirm if antiretroviral therapy could indeed prevent HIV transmission. I recall presenting to healthcare workers at the local public hospital, who were preparing to undertake this vital study.
**Option 4 (Emphasizing the future impact):**
> The success of HIV management produced an unexpected challenge: Longer periods of infectivity meant a growing epidemic. In 2010, while working with the CDC on HIV prevention in Kenya, I was involved in a significant multinational study. This research explored a revolutionary concept: using anti-HIV treatment as a tool to stop transmission. In a conference room at the local public hospital, I was tasked with informing the healthcare workers who would be on the front lines of this critical study.
Here are a few paraphrased options, each with a slightly different emphasis:
**Option 1 (Focus on Sacrifice and Dedication):**
> The vast majority of the dedicated individuals on our research team were women, earning a modest salary of approximately $300 per month. These were our crucial community health workers, drawn from a population facing an alarmingly high HIV infection rate – one in four women in their age bracket. At the time, access to life-saving antiretroviral therapy was severely constrained by both cost and logistical challenges, with only a third of those requiring treatment actually receiving it. This stark reality meant that the women I spoke with carried the heavy burden of knowing that many they served were destined for the same fate as those succumbing to AIDS in San Francisco wards. Despite this grim outlook, they persevered, venturing into remote villages to meticulously enroll study participants and return with vital data.
**Option 2 (Focus on the Stark Reality and Unwavering Commitment):**
> Our study workforce, overwhelmingly comprised of women, was compensated at the standard rate of about $300 monthly. These women hailed from a community disproportionately affected by HIV, where one in four women of their age group were infected. The availability of anti-HIV medication was a significant hurdle, both financially and logistically, with a mere third of those needing treatment actually obtaining it. This dire situation cast a long shadow, implying that an indeterminate number of the women we interviewed would tragically face the same outcome as AIDS patients in San Francisco’s hospitals. Nevertheless, they embarked on arduous journeys to villages, diligently recruiting participants and gathering essential data for our research.
**Option 3 (More Concise and Direct):**
> The research team was predominantly composed of women, earning a standard salary of around $300 per month. They served as our community liaisons, originating from an area with a critical HIV prevalence: one in four women in their age group tested positive. Antiretroviral medication was difficult to access due to financial and logistical barriers, meaning only one-third of those who needed it received care. Consequently, many of the women participating in our study were likely to die from AIDS, mirroring the tragic epidemic in San Francisco. Despite these bleak realities, they traveled to villages, undertaking the demanding work of enrolling participants and collecting study data.
**Key Changes and Why:**
* **”Almost all were women”**: Paraphrased to “The vast majority of the dedicated individuals on our research team were women,” “Our study workforce, overwhelmingly comprised of women,” or “The research team was predominantly composed of women” for variety and a slightly more formal tone.
* **”standard princely salary of about $300 a month”**: Changed to “modest salary of approximately $300 per month,” “standard rate of about $300 monthly,” or “standard salary of around $300 per month.” “Princely” is often ironic when referring to low wages, so using “modest” or simply stating the amount emphasizes the contrast with the risk.
* **”study workers because they came from the community most at risk”**: Reworded to “crucial community health workers, drawn from a population facing an alarmingly high HIV infection rate,” “community liaisons, originating from an area with a critical HIV prevalence,” or similar to explain their role and the reason for their inclusion more fluidly.
* **”One-in-four women in their age group were HIV infected”**: Rephrased for flow and impact, e.g., “where one in four women of their age group were infected.”
* **”Access to anti-HIV medication was fiscally and logistically limited. Only a third of those who needed treatment actually received it.”**: Combined and reworded for better sentence structure and stronger vocabulary like “severely constrained by both cost and logistical challenges” or “significant hurdle, both financially and logistically.”
* **”That meant an unknown number of the women to whom I was speaking were ultimately going to die the same death as those in the San Francisco AIDS ward.”**: This is a powerful sentence, so the paraphrases aim to retain its emotional weight while rephrasing. Options include “This stark reality meant that the women I spoke with carried the heavy burden of knowing that many they served were destined for the same fate,” or “This dire situation cast a long shadow, implying that an indeterminate number of the women we interviewed would tragically face the same outcome.”
* **”But they went out to the villages and did the hard work to enroll study subjects and bring home the data.”**: Transformed into more active and descriptive phrases like “persevered, venturing into remote villages to meticulously enroll study participants and return with vital data,” or “embarked on arduous journeys to villages, diligently recruiting participants and gathering essential data.”
A groundbreaking 2016 scientific study, heavily influenced by the contributions of women worldwide, revolutionized the understanding of HIV. This landmark research, which has since become one of the most cited in medical history, unequivocally proved that HIV transmission is not an unavoidable outcome. The study demonstrated a powerful truth: the chain of infection can be definitively broken by implementing effective anti-HIV treatment, leading to zero transmission when individuals receive the appropriate care.
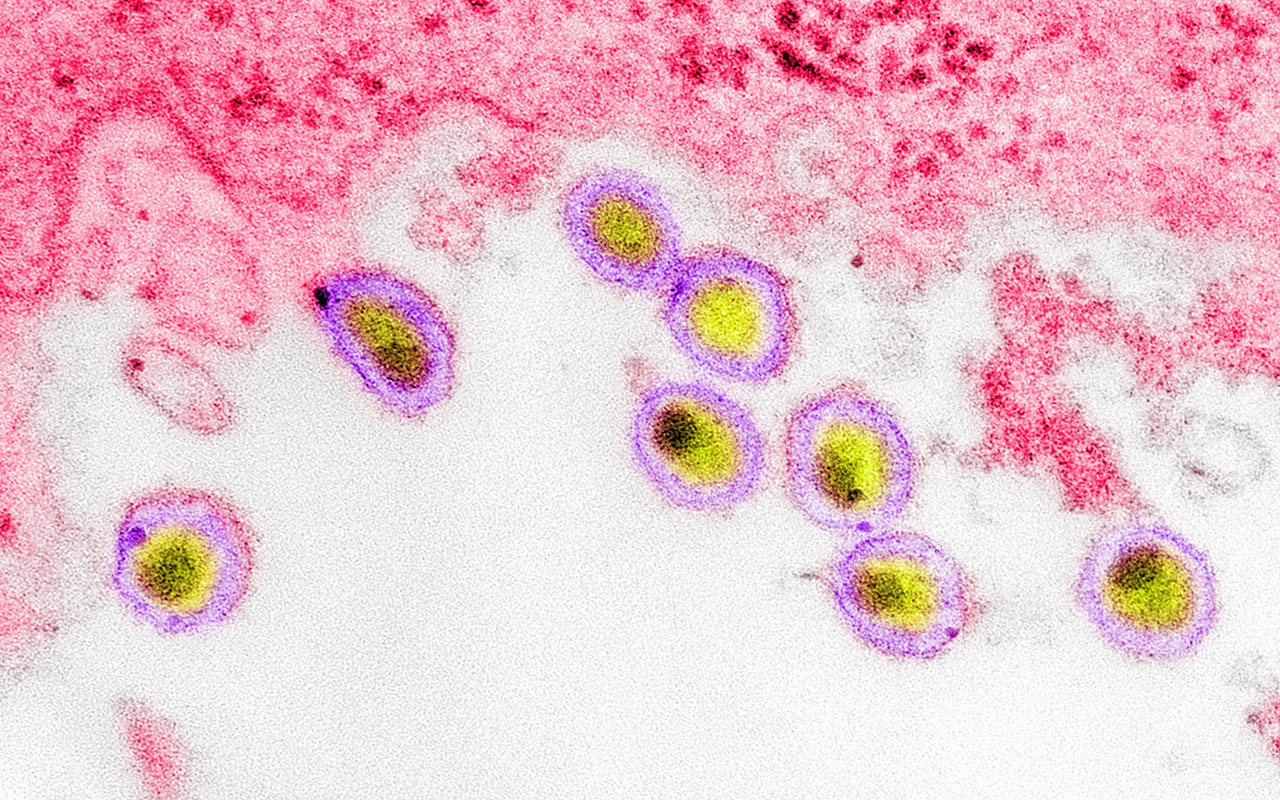
Ten years later, Robert F. Kennedy Jr. has voiced skepticism regarding the established understanding of HIV, proposing a theory that individuals with ulterior motives orchestrated a diversion from other potential causes of AIDS, such as “toxins.” Furthermore, he has asserted, without providing supporting evidence, that anti-HIV drug trials were conducted on fraudulent and unethical grounds, leading to fatalities.
The year 2025 marked a period of profound upheaval for the Centers for Disease Control and Prevention’s (CDC) Division of HIV Prevention, as a series of drastic measures reshaped its operations and public information.
Five of the division’s eleven branches were abolished, resulting in significant employee layoffs. Concurrently, all of the CDC’s HIV-related websites were taken offline. Although later restored by court order, critical pages reappeared with highly controversial disclaimers.
For instance, the web page dedicated to HIV treatment now prominently features a header stating: “This page does not reflect biological reality and therefore the Administration and this Department rejects it.” A similar disclaimer appeared on the HIV prevalence page, though an anonymous CDC employee reportedly managed to insert an explanation for the data being frozen in 2023: “the branches that produced HIV incidence estimates… were eliminated.”
Further impacting public health efforts, presidential candidate RFK Jr. canceled $759 million in HIV research grants. He additionally proposed a radical restructuring that would transfer all responsibility for HIV from the CDC and other agencies to a new “Administration for a Healthy America,” operating under his direct control and facing an 80% reduction in funding. While this reorganization remained pending, a separate proposal for a half-billion-dollar cut to HIV treatment budgets was put before Congress.
At a pivotal moment when the definitive tools to conquer the HIV epidemic appeared to be within reach, extraordinary progress was evident. New infections had been slashed by more than 90%, and in a monumental public health victory, the transmission of the virus from mother to child had been completely eliminated.
Facing severe financial strain, states are increasingly compelled to scale back, rather than fully fund, essential healthcare initiatives. Across the nation, various expenditure reduction measures are either being implemented or are under serious consideration.
These drastic cutbacks include establishing waiting lists for critical medical treatments, narrowing the range of available prescription drug options, imposing new work requirements for benefit eligibility, and tightening income thresholds for access to services. Perhaps most critically, some states are discontinuing reimbursement for vital laboratory assays—tests crucial for monitoring patient response and ensuring the efficacy of prescribed medications.
Globally, the trend of defunding HIV prevention is a growing concern, exacerbated by the U.S.’s decision to withdraw critical assistance from international programs. This international retrenchment, coupled with the erosion of domestic safeguards against the virus and a heightened vulnerability to foreign exposures, sets the stage for a significant acceleration in viral spread.
Such a scenario would inevitably see infection rates climb far beyond the current estimate of one in 300 Americans. Each new case would then serve as a catalyst for further transmission, creating a dangerous feedback loop. The inevitable consequence, experts warn, is that HIV will breach its traditionally recognized risk groups, evolving into a generalized pandemic across the United States.
After nearly five decades of relentless dedication from AIDS activists in San Francisco, village health workers in Kenya, and laboratorians across the globe, a critical choice now stands before humanity regarding the HIV epidemic.
With the widespread application of effective treatment, the path is clear: we can contain and eventually halt the epidemic, preventing its escalation into a devastating global pandemic. This not only allows those living with HIV to lead near-normal, productive lives but also delivers substantial cost savings for society.
Conversely, a failure to prioritize and provide comprehensive treatment portends a grim future. This inaction risks uncontrolled transmission, an unchecked epidemic spiraling into a pandemic, leading to untold suffering, premature deaths, and immense financial and human costs for societies worldwide.
For public health, the year 1983 carries a stark significance, mirroring the dystopian warnings George Orwell famously gave to politics with “1984.” When confronting HIV, the critical question arises: Do we truly wish to regress to the profound despair and helplessness that characterized that early era of the epidemic?
The alternative is a proactive and determined stand. By harnessing robust scientific advancements and powerful advocacy, we possess the capacity to restore our defenses and defy any such grim inevitability. The imperative is clear: to halt any potential HIV resurgence before it can gain momentum, thereby ending the epidemic decisively and preventing its escalation into a devastating global pandemic.
Live Science Opinion offers a compelling look at the critical scientific issues shaping our world, delivered by leading experts and renowned scientists. These articles provide valuable perspectives on topics that directly impact you and the global community.







