More than a decade ago, on a sweltering Saturday, an eight-year-old boy was rushed to a San Antonio hospital in a critical, unresponsive state. For days, he had suffered from a high fever, debilitating headaches, persistent vomiting, and acute sensitivity to light. His mother, residing near the Texas-Mexico border, had previously sought help at various clinics across Mexico, but his condition had only worsened. By the time he reached the emergency room, the young patient was deeply unconscious, showing no reaction to sound, light, or any other stimuli.
Faced with a critically ill child, doctors placed him on a ventilator and launched an intense, urgent investigation into his deteriorating condition. The shocking revelation came from a sample of the boy’s cerebrospinal fluid: *Naegleria fowleri*, the dreaded “brain-eating amoeba,” an organism whose discovery typically extinguishes nearly all hope for survival.
For Dr. Dennis Conrad, a pediatric infectious disease specialist then practicing at University Hospital in San Antonio, this particular instance marked only the third such case he had encountered in his entire career. The gravity of the situation was compounded by a stark reality: both of his previous patients afflicted with the condition had tragically succumbed.
Conrad, upon learning of miltefosine’s recent approval as an experimental treatment for N. fowleri infections, swiftly integrated the drug into the boy’s existing medical regimen. This new addition complemented a treatment plan already comprising a range of antimicrobial and anti-inflammatory medications.
Characterizing the illness as “formidable,” Conrad told Live Science that its severity mandates an aggressive, “no-holds-barred” therapeutic strategy, deploying every conceivable treatment option available.
Upon arrival in San Antonio, the child faced a grim medical prognosis, having already battled illness for five days. This timeline was particularly critical, as infections with *N. fowleri* are notoriously swift and devastating, typically proving fatal within approximately five days of symptom onset. The extreme lethality of the disease is starkly reflected in data from the Centers for Disease Control and Prevention (CDC): between 1962 and 2022, the United States documented 157 confirmed human cases of *N. fowleri* infection, with a harrowing four individuals surviving.
Globally, the situation mirrors this grim reality. Infections with this particular amoeba are uncommon, and fatalities are exceedingly high. However, a handful of individuals who have recently survived this devastating illness may have the drug miltefosine to thank. This medication is now the most recently endorsed treatment for primary amebic meningoencephalitis (PAM), the severe brain infection caused by the amoeba. Furthermore, promising new drug developments are on the horizon. The critical challenge lies in whether these treatments can be administered effectively to patients before irreversible damage occurs.
Here are a few paraphrased options, each with a slightly different emphasis:
**Option 1 (Focus on the threat):**
> The microscopic organism *Naegleria fowleri*, often dubbed the “brain-eating amoeba,” flourishes in warm freshwater environments, typically preferring temperatures around 80°F (26.6°C) or higher. While it can survive in cooler conditions, its optimal habitat is crucial for its proliferation. Infection occurs solely by chance, when contaminated water is propelled into the nasal passages. This invasive route allows the amoeba to breach the cribriform plate, a delicate bone structure, and travel directly to the olfactory nerve, which then serves as a pathway into the brain.
**Option 2 (Focus on the mechanism of infection):**
> *Naegleria fowleri* finds its ideal home in warm freshwater, thriving in temperatures of 80°F (26.6°C) and above, though it may persist in cooler waters according to the CDC. This dangerous amoeba infects humans through an unfortunate accident: water forced into the nose. This influx carries the organism through the cribriform plate, a porous bone, and directly to the olfactory nerve, essentially opening a direct route for the amoeba to reach the brain.
**Option 3 (More concise and direct):**
> Thriving in warm freshwater above 80°F (26.6°C), *Naegleria fowleri* poses a rare but serious threat. Infection is unintentional, occurring when water is driven up the nose, allowing the amoeba to traverse the cribriform plate and reach the olfactory nerve. This nerve acts as a direct conduit, transporting the organism to the brain.
**Key changes made and why:**
* **Replaced “thrives”**: Used words like “flourishes,” “finds its ideal home,” and “thriving” for variety.
* **Clarified “warm fresh water”**: Added context like “environments” and “habitat.”
* **Described *N. fowleri***: Used “microscopic organism” and “brain-eating amoeba” to provide more descriptive language.
* **Paraphrased “might manage to hang on”**: Used “may persist” or “can survive” for a more formal tone.
* **Changed “infects people purely by accident”**: Rephrased to “occurs solely by chance,” “infects humans through an unfortunate accident,” or “infection is unintentional.”
* **Explained “forced up the nose”**: Used “propelled into the nasal passages” or “driven up the nose.”
* **Described “lacy bone called the cribriform plate”**: Used “delicate bone structure,” “porous bone,” or simply “cribriform plate” while explaining its function (breaching, traversing).
* **Clarified “olfactory nerve, which acts as a highway to the brain”**: Used “pathway to the brain,” “direct route,” or “direct conduit.”
* **Journalistic Tone**: Employed more formal vocabulary, clear sentence structure, and focused on factual reporting.
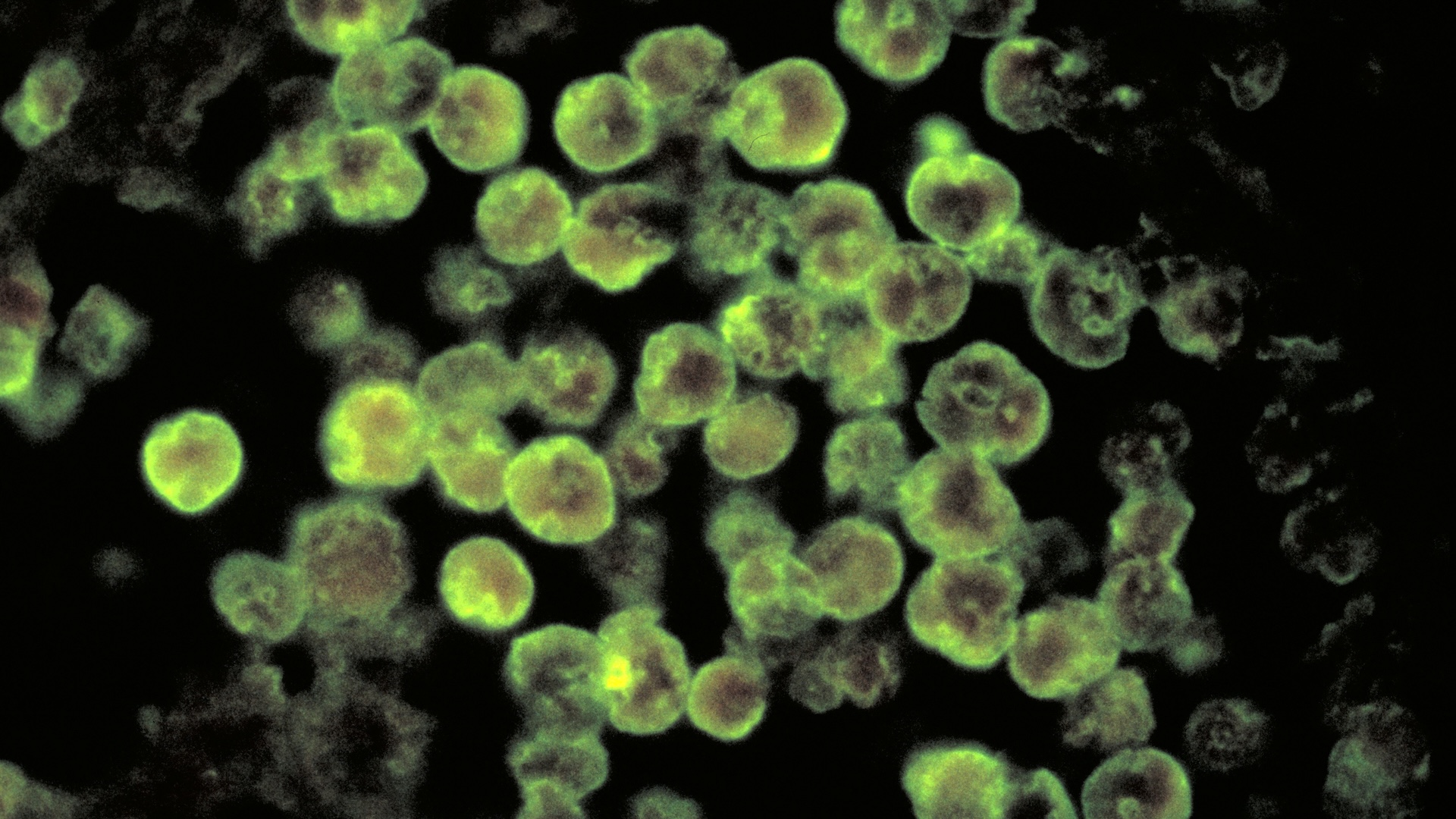
Individuals with weakened immune systems face a significantly elevated risk from this particular infection, according to Dr. Juan Fernando Ortiz, a neurology resident at Corewell Health in Grand Rapids, Michigan, and author of a journal article detailing treatment approaches.
Data from the CDC indicates that boys under the age of 14 represent a disproportionately large segment of reported cases. Researchers suggest this may be attributed to their higher propensity for activities that can propel water into the nasal passages, such as jumping and diving.
While the majority of infections stem from exposure to natural bodies of water, rare instances have been connected to treated water sources, including splash pads. Furthermore, a small number of individuals have contracted the infection through the use of tap water in nasal rinsing devices like neti pots.
In August 2013, Dr. Conrad and his team encountered a young patient whose story of infection was unfortunately all too common. The child had spent the summer months at a makeshift camp situated along the Rio Grande, an area lacking basic amenities like running water. During their stay, residents, including the child, would bathe in the river, and the youngster particularly enjoyed playing in the shallow areas.
The most probable scenario is that this is where the child contracted the amoeba, a dangerous organism that Conrad and his team were now racing against time to eliminate, fearing it could inflict irreversible damage beyond the child’s ability to endure.
Here are a few paraphrased options, maintaining a journalistic tone and focusing on uniqueness and engagement:
**Option 1 (Focus on the dual nature of the attack):**
> The deadly pathogen known as PAM, or Primary Amebic Meningoencephalitis, unleashes its destruction through a two-pronged assault on the brain. While the amoeba itself directly consumes vital brain tissue – earning it the grim “brain-eating” label – a significant portion of the catastrophic damage actually stems from the body’s own overzealous immune system. Dr. Conrad elaborated that this aggressive immune reaction is a misguided defense against an unwelcome invader within the central nervous system. Typically, parasites that establish themselves within a host develop sophisticated mechanisms to suppress the immune response, ensuring their continued survival. However, *Naegleria fowleri*, the amoeba responsible for PAM, has no evolutionary need for a host and consequently lacks these immune-evading adaptations. “It acts like a bull in a china shop,” Dr. Conrad characterized, highlighting its destructive, unrefined approach.
**Option 2 (More concise and direct):**
> PAM inflicts fatal damage on the brain through overwhelming tissue destruction. The amoeba’s direct assault earns it the notorious “brain-eating” title, but Dr. Conrad explained that the body’s vigorous immune response to this foreign entity plays a significant role in the ensuing brain damage. Unlike parasites that evolve to coexist within a host by dampening immune reactions, *Naegleria fowleri* has no such adaptations. “It’s a bull in a china shop,” Conrad stated, emphasizing the amoeba’s unhindered destructive capacity due to its lack of host-specific evolutionary adaptations.
**Option 3 (Emphasizing the body’s role in its own demise):**
> The devastating impact of PAM on the brain is a result of massive tissue destruction, a process exacerbated by the body’s own defenses. While the amoeba *Naegleria fowleri* contributes to the damage directly, leading to its “brain-eating” moniker, Dr. Conrad highlighted that the body’s aggressive immune response to the intruder is a major driver of the fatal brain injury. Parasites that have evolved to inhabit a host typically possess strategies to quiet the immune system, but *N. fowleri* lacks these adaptations because it has no need for a long-term host. “It’s a bull in a china shop,” Conrad commented, underscoring the amoeba’s unmitigated destructive power in the absence of evolutionary controls.
Each option aims to rephrase the original while retaining the core information about PAM’s destructive mechanisms, the role of the immune system, and the amoeba’s lack of host-specific adaptations, using varied sentence structures and vocabulary.
The Centers for Disease Control and Prevention (CDC) reports that infections from the brain-eating amoeba *Naegleria fowleri* remain rare in the United States, with annual cases typically ranging from zero to six. Dr. Julia Haston, a medical epidemiologist with the CDC’s Waterborne Disease Prevention Branch, noted that there is no indication of an increase in these infections.
While the majority of cases have historically been concentrated in southern states like Texas and Florida, recent years have seen a notable uptick in occurrences further north. Dr. Haston suggests that this geographical shift may be linked to climate change, as warming water temperatures create more favorable conditions for the amoeba. Supporting this observation, a 2021 study identified a rise in cases within the Midwest, extending as far north as Minnesota.
To err on the side of caution for those concerned about potential exposure, the recommended strategy is to operate under the assumption that the amoeba Naegleria fowleri is present in all natural freshwater sources, including lakes and rivers. This was the advice given by Haston.

In a critical fight against a brain-invading amoeba affecting a San Antonio patient, Dr. Conrad and his team deployed a cutting-edge therapy: miltefosine. This antimicrobial agent, initially developed to combat leishmaniasis, a disease transmitted by a tropical parasite, had demonstrated encouraging results against *Naegleria fowleri* in prior research. Consequently, the CDC had begun supplying it for Primary Amebic Meningoencephalitis (PAM) cases. According to Dr. Ortiz, a key advantage of miltefosine is its ability to cross the blood-brain barrier and its generally favorable patient tolerance. This is a significant benefit, as he noted, many antiparasitic medications can also harm human cells.
Here are a few options for paraphrasing the text, maintaining a journalistic tone:
**Option 1 (Focus on speed and source):**
> A critical medication, now commercially known as Impavido, was dispatched by the CDC and reached the child just 14 hours after their hospital admission.
**Option 2 (Highlighting the commercial availability first):**
> While today available commercially as Impavido, the life-saving drug was specifically ordered from the CDC by physicians and arrived 14 hours after the child’s admission.
**Option 3 (More concise):**
> Doctors secured the drug, commercially recognized as Impavido, through an order with the CDC. It was delivered 14 hours post-admission.
**Option 4 (Emphasizing the urgency):**
> In a race against time, doctors obtained the drug – now marketed as Impavido – from the CDC. It arrived at the hospital a mere 14 hours after the child was admitted.
The child survived.
Nevertheless, the experience left an indelible mark. Upon his discharge from the hospital, the boy’s capabilities were severely limited; he could breathe independently, but his other faculties remained significantly compromised. Despite months of intensive rehabilitation, which allowed him to reclaim some abilities, his family continued to provide essential assistance for basic self-care, Conrad confirmed.
That same summer, in a rare medical triumph, a 13-year-old girl in Arkansas defied the near-certain fatality of a brain-eating amoeba infection. After contracting the deadly *Naegleria fowleri* from an artificial pond, she received swift and aggressive treatment, crucially including the drug miltefosine. Her remarkable recovery, detailed in a 2015 case report, culminated in six months of rehabilitation, after which she exhibited no lingering neurological effects from her harrowing encounter.
Before recent breakthroughs, she and a young patient from Texas held the distinction of being the first U.S. survivors of Primary Amebic Meningoencephalitis (PAM) since 1978, marking a significant medical rarity. Their remarkable recovery was later joined by another success story in 2016, when a 16-year-old boy in Florida, after contracting PAM and receiving treatment with the drug miltefosine, also made a full recovery.
Despite the introduction of miltefosine as a therapeutic option, the fight against Primary Amebic Meningoencephalitis (PAM) remains devastatingly difficult. Not all patients treated with the drug have survived, underscoring the disease’s profound lethality. According to data from the Centers for Disease Control and Prevention (CDC), even with miltefosine, PAM continues to claim lives at an overwhelming rate, with its fatality hovering stubbornly above 97%.
Annually, with the advent of summer, a limited number of new Primary Amebic Meningoencephalitis (PAM) cases emerge across the nation. As these rare but devastating infections surface, medical professionals are relentlessly pursuing improved therapeutic interventions.
One promising frontier involves therapeutic hypothermia, a strategy gaining increased attention. According to Conrad, doctors are exploring the controlled cooling of patients’ core body temperature to approximately 95°F (35°C). This approach is particularly compelling given research suggesting it may significantly enhance neurological recovery following severe brain trauma.
The horizon for new pharmaceutical solutions may soon broaden, a critical advancement given the drawbacks of current treatments. For example, Miltefosine, a drug that could offer promise, is severely limited by its toxic effects on the kidneys and liver, and remains largely inaccessible in developing nations. This insight comes from Jacob Lorenzo-Morales, a senior lecturer in parasitology and director of the University of La Laguna Institute of Tropical Diseases and Public Health of the Canary Islands.
**New Hope in the Fight Against Brain-Eating Amoebas: Nitroxoline Emerges as a Promising Therapeutic**
Researchers, led by Dr. Lorenzo-Morales, are actively pursuing novel treatments for infections caused by the deadly brain-eating amoeba, *Naegleria fowleri*. Among the most encouraging candidates is nitroxoline, an antibiotic already approved for use in Europe to combat urinary tract infections.
Published in the journal *Antibiotics* in August 2023, a study by Lorenzo-Morales and his team demonstrated that low doses of nitroxoline effectively triggered cell death in *N. fowleri* within laboratory settings. Crucially, these concentrations did not exhibit toxicity to human host cells.
This groundbreaking research is further bolstered by the drug’s prior success in treating a patient infected with *Balamuthia mandrillaris*, another dangerous amoeba affecting the brain. This suggests nitroxoline’s potential as a broad-spectrum therapeutic agent against these devastating parasitic infections.
The therapeutic potential of Nitroxoline is currently being explored through ongoing animal studies. Researchers anticipate unveiling positive findings at next year’s international Free-Living Amoebae Meeting, the prominent biannual gathering for specialists in amoebic diseases.
According to Lorenzo-Morales, Nitroxoline, already globally available and possessing existing regulatory approvals for other conditions, benefits from a significantly streamlined development path. This pre-existing approval, he noted, circumvents the necessity for lengthy, extensive clinical trials, potentially allowing medical professionals to begin prescribing the drug off-label without significant delay.
Beyond current treatments, significant research is underway to identify novel pharmaceutical interventions for Primary Amebic Meningoencephalitis (PAM). A particularly innovative area of focus involves the potential development of mRNA vaccines designed to combat *Naegleria fowleri* infections. Illustrating this cutting-edge pursuit, a 2024 study published in the journal *Scientific Reports* utilized sophisticated modeling techniques to analyze the amoeba’s surface features, offering preliminary insights into the potential design of such a vaccine. (Attempts by Live Science to reach the study’s authors for an interview were unsuccessful.)
Scientists led by Lorenzo-Morales are broadening their investigations, now focusing on the therapeutic potential of elatol, a distinctive pigment sourced from red algae.
According to Lorenzo-Morales, the research has already yielded promising results. His team has successfully isolated crucial compounds from the algae that demonstrate remarkable potency against various free-living amoebas, including the dangerous *Naegleria*. These compounds, he added, prove effective at concentrations significantly lower than those currently utilized in conventional treatments.
While current research shows promise in laboratory settings, the crucial leap to human testing remains contingent on securing significant financial backing from pharmaceutical companies.
This advancement presents a considerable hurdle, as noted by Lorenzo-Morales. He explains that drug manufacturers often hesitate to invest heavily in what they perceive as a “rare” disease like PAM, citing limited potential for profit. However, Lorenzo-Morales contends that PAM’s true prevalence is likely much higher than currently acknowledged. He argues that the disease frequently goes undiagnosed or unrecognized, suggesting that the actual market for effective treatments could be substantially larger than pharmaceutical executives currently believe.
For patients confronting Primary Amoebic Meningoencephalitis (PAM), the most critical immediate hope hinges on significantly expediting diagnosis. The window for effective intervention against PAM is exceptionally narrow, cautioned Julia Walochnik, a professor of tropical medicine at the Medical University of Vienna who specializes in amoebic diseases. Walochnik underscored the dire prognosis in an interview with Live Science, stating, “If it’s too late, it doesn’t matter which drug is used; the patient will usually not survive,” highlighting that delayed recognition invariably renders medical treatments futile.
Delayed medical intervention is being considered as a potential explanation for the profound brain damage sustained by an 8-year-old patient under Conrad’s care. This tragic outcome stands in stark contrast to the more complete recoveries observed in other young individuals who received treatment during the same timeframe.
Diagnosing a rare and often fatal brain infection caused by an amoeba hinges on a straightforward laboratory test: identifying microscopic, single-celled organisms swimming in cerebrospinal fluid. However, the urgency to order this specific test can be delayed because the initial symptoms of Primary Amebic Meningoencephalitis (PAM) closely mimic more prevalent conditions like viral or bacterial meningitis.
To combat this diagnostic hurdle, families who have tragically lost children to PAM are actively campaigning to elevate public and medical awareness. Their efforts aim to promote earlier identification and intervention, potentially saving lives. A prime example is the Jordan Smelski Foundation for Amoeba Awareness, established by the parents of an 11-year-old boy who succumbed to PAM in 2014. This foundation actively organizes educational initiatives targeting both healthcare professionals and the general public.
Here are a few paraphrased options, maintaining a journalistic tone and conveying the original meaning:
**Option 1 (Focus on Speed of Diagnosis):**
> “Increased awareness has significantly accelerated the diagnostic process, according to Lorenzo-Morales. He notes that in the past four to five years, clinical cases have consistently seen swift diagnoses – a stark contrast to previous experiences.”
**Option 2 (Highlighting the Shift):**
> Lorenzo-Morales observed a tangible impact from heightened awareness, stating that “in the last four to five years, every clinical case we’ve encountered has led to a rapid diagnosis. This is a considerable change from how things were before.”
**Option 3 (More Concise):**
> The growing understanding of a particular issue has led to faster diagnoses in clinical cases over the last four to five years, a trend Lorenzo-Morales highlighted as a marked improvement over the past.
**Option 4 (Emphasizing the “Before and After”):**
> Lorenzo-Morales attributes the recent speed of diagnosis in clinical cases to increased awareness. “What we’re seeing now, with rapid diagnoses in every case over the past four to five years, simply did not happen previously,” he explained.
**This report was first published on July 26, 2024.**
**Test Your Neurological Prowess: A Quiz to Uncover Your Brain’s Secrets**
How well do you truly understand the intricate organ that governs our every thought, feeling, and action? Dive into our engaging quiz and put your knowledge of the human brain to the ultimate test. Prepare to explore the fascinating complexities of this remarkable biological marvel!






